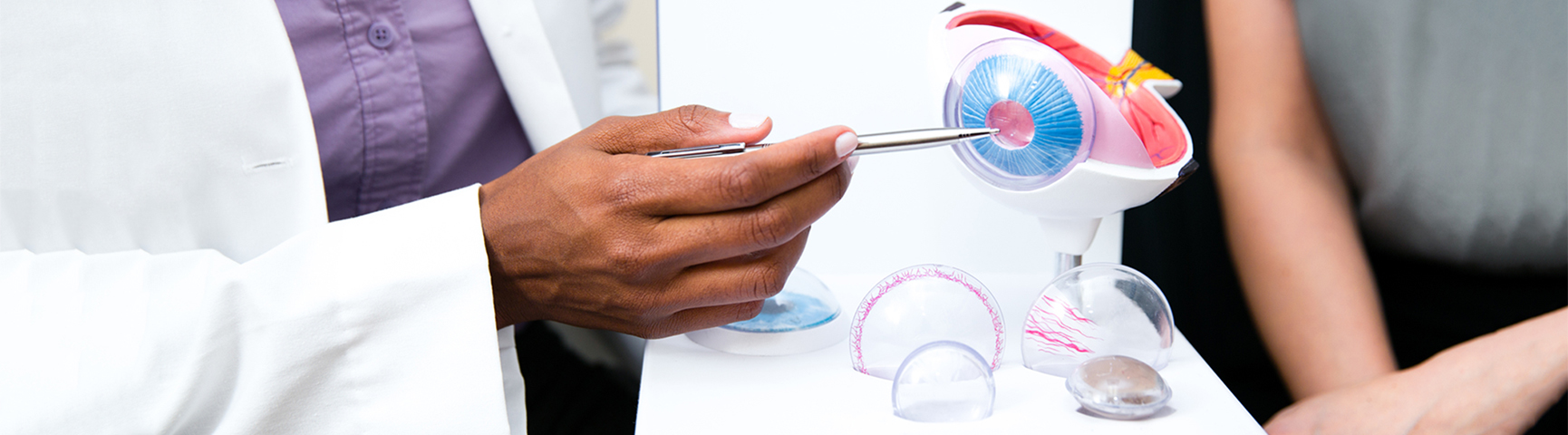
Explore these topics to learn more about some of the eye conditions that we commonly treat. As an informed patient, you will feel more comfortable with any treatments or services you might require.
The complex systems of the eye can sometimes be affected by genetic, biological, or environmental factors. Learn more about some of these common eye conditions by clicking on the condition names.

Myopia
Myopia, or near-sightedness, is when the eye cannot see clearly at the distance, but can see well up close. This happens when the length of the eye is too long or if the curvature of the cornea is too steep, causing the light rays to be focused in front of the retina. Ways to correct for myopia include glasses, contact lenses, and refractive surgery (LASIK, PRK, phakic lens implant)
Hyperopia
Hyperopia, or far-sightedness, is when the eye sees better at the distance than up close. This happens when the length of the eye is too short or if the curvature of the cornea is too flat, causing the light rays to be focused behind the retina. Our natural lens can sometimes compensate for this by accommodation, but as we age, we start to lose this ability of auto-focus. Ways to correct for hyperopia include glasses, contact lenses, and refractive surgery (LASIK, PRK)
Astigmatism
Astigmatism means that instead of focusing the light to a single point, the eye focuses the light to multiple different locations. This is either caused by an irregular, (football shaped) cornea, or irregularities in the natural lens inside the eye. Astigmatism can exist in combination with any other refractive disorders. Ways to correct for astigmatism include glasses, contact lenses, and refractive surgery (LASIK, PRK)
Presbyopia
Presbyopia happens to all of us around the age of 45. As we age, the natural lens begins to harden and gradually lose its ability to change in shape. This makes it more difficult to focus on objects up close. Initially, affected individuals can notice this by needing to hold their reading material further away. Some near-sighted individuals find it helpful to take their glasses off to read. Presbyopia may be corrected with glasses, contact lenses, monovision LASIK/PRK, and lens extraction with implantation of presbyopia correcting lenses.
Cataract
A cataract is a yellowing or clouding of the natural clear lens inside the eye, which causes the vision to decrease. This is a normal aging process and happens to everyone. Certain disease processes, including diabetes and inflammation within the eye can speed up the formation of a cataract. A cataract is problematic when it decreases the vision enough to affect your daily activities, such as driving and reading. Changing your glasses prescription may partially improve your vision, but the vision is typically still impaired since the eye is seeing through a cloudy lens. Cataract surgery is then needed to remove the cloudy lens, and a clear lens implant is placed to restore the vision.
Glaucoma
Glaucoma is a disease of the nerve of the eye responsible for transmitting vision from the eye to the brain. The damage to the nerve typically causes the eye to lose its peripheral vision. As the nerve damage worsens, the loss of peripheral vision becomes more and more central, and can eventually lead to blindness. Glaucoma is usually associated with high eye pressure, but even individuals with normal eye pressure can develop glaucoma. The high eye pressure that causes glaucoma does not produce any eye symptoms most of the time. This is why regular complete eye exams are essential for the early diagnosis and treatment of glaucoma.
Diabetic Retinopathy
Patients with diabetes are at increased risk of vision loss from changes in the retina. The increase in blood sugar causes damages to the blood vessels in the retina, which can cause swelling, bleeding, abnormal blood vessel formation, and scarring in the retina. All these changes can cause permanent damage to the retina and decrease vision, leading to blindness in advanced cases. The most important treatment of diabetic retinopathy is tight control of the blood sugar. Regular dilated eye exams are essential in the early detection of any damages in the retina. Laser treatments may be indicated in certain cases to try to slow down the progression of the damage.
Posterior Vitreous Detachment
Posterior Vitreous Detachment (PVD) is a common condition that causes the symptom of floaters. The floater is basically a clumping of the collagen substance in the back portion of the eye. While the floater itself is not harmful to the eye, the process of developing the floaters can cause retinal tears or even retinal detachment. It is important to have a complete dilated eye exam when new floaters are seen to ensure there is no problems with the retina. There is no good treatment to get rid of the floaters, but the brain tends to gradually ignore their presence with time.
Retinal Tear and Detachment
Retinal tear and detachment can lead to permanent vision loss if not diagnosed and treated promptly. Classic symptoms of retinal tear and detachment include flashes of light in the eye, prominent floaters, or a curtain-like shadow covering part of the vision. Many retinal detachment starts as a small tear in the retina. If a retina tear is diagnosed early enough, it can be treated with a laser procedure to prevent development of retinal detachment. If retinal detachment is present, you will be referred to a retinal specialist for urgent repair.
Age Related Macular Degeneration
Age related macular degeneration is the leading cause of central vision loss in patients over the age of 50 in the United States. It basically represents aging changes in the macula, which is the central part of the retina that is responsible for your central vision. Macular degeneration comes in two forms, dry and wet. Dry macular degeneration is less aggressive and slowly progressive, but can still result in advanced damage to your vision. Wet macular degeneration is much more aggressive and can result in significant permanent vision loss if not diagnosed and treated promptly. Early changes of macular degeneration do not always come with symptoms, so it is essential to schedule a routine eye exam.
Dry Eyes
Dry eye syndrome is a very common condition that affects millions of patients and can cause a wide variety of chronic eye symptoms, which can include burning, itching, eye fatigue, redness, tearing, blurred vision, foreign body sensation, and eye pain. There are many different causes that contribute to dry eye syndrome and the treatment can vary depending on the exam findings. Although it can seem like a minor problem, dry eye syndrome that is untreated can cause permanent damage to the eyes. It is important to have a detailed eye exam to determine what treatment is best suited for the specific findings.
Blepharitis
Bphepharitis means inflammation of the eyelids. The Meibomian glands, or oil glands of the eyelids produce an essential layer to the tear film that keeps the tears from evaporating too quickly. Blepharitis causes dysfunction of the Meibomian gland and can lead to dry eye syndrome and eye irritation, redness, and crusting of the eyelashes. The treatment of this chronic condition relies tremendously on the patient. Warm compress and lid scrubs can help in most cases. In more advanced cases, medication eye drops or pills are needed to control the inflammation.
Pterygium
A pterygium is a wing shaped growth over the cornea of the eye, usually found towards the nose. It represents damage to the outside layer of the eye from harmful UV rays from sunlight exposure. Pterygium can progressively enlarge and cause symptoms of eye irritation, astigmatism, decreased vision, and chronic eye redness. Surgical excision is a good option for symptomatic cases. A specialized technique of excision is needed to prevent recurrence of the pterygium.
Keratoconus
Keratoconus means cone shaped cornea. It affects 1/2000 of the population by gradually changing the shape of the cornea to an irregular cone shape. This irregular shape affects how the cornea refracts light and causes poor vision. The vision in early cases can be corrected by glasses or contact lenses. As the cone progresses, the increased irregularity becomes too significant for glasses or contact lenses to correct. The cone can be so severe that a contact lens will not stay on the eye. Surgical management of keratoconus involves intracornea ring segments, or INTACS, and corneal transplantation. Recent advances in corneal collagen crosslinking under FDA investigation is an exciting new treatment for keratoconus that is on the horizon.
Chalazion
A chalazion, commonly referred to as a stye, is a small, non-infectious bump that develops in the upper or lower eyelid due to blockage of the Meibomian gland. The Meibomian glands line the margins of our eyelids and produce the oily layer of our tear film that lubricates the eye.
A chalazion can often be resolved with warm compression. Antibiotics generally do not help with a chalazion unless there is an associated infection. If the chalazion does not resolve with conservative treatments, a drainage procedure can be performed.

A cataract is when the natural lens of our eyes become cloudy or discolored, causing blurry vision and decreased quality of vision.
Does everyone get cataracts?
Cataracts develop as a normal process of aging, and generally start producing visual symptoms in our 50s and 60s. The cataracts usually worsen very slowly and many people become used to the suboptimal vision, not knowing their vision is no longer normal.
When should I have cataract surgery?
We recommend cataract surgery when the vision is bothersome even when the best glasses or contacts are worn. When activities of daily living become difficult to perform, like driving and reading, it may be time to consider cataract surgery.
Is cataract surgery painful?
Cataract surgery is an outpatient procedure that is done one eye at a time, usually a couple of weeks apart. The procedure is not painful, and the recovery is fast. Patients are generally relieved about how easy the whole process is after experiencing cataract surgery.
Is cataract surgery done by laser?
The majority of cataract surgeries are done without the use of a laser. However, Laser-Assisted Cataract Surgery is an exciting technology that is available to our patients. We will discuss with you the many benefits of Laser-Assisted Cataract Surgery at your visit.
Does insurance cover cataract surgery?
Cataract surgery is a procedure that is covered by medical insurance, and is subject to the insurance plan’s co-pay and deductible. Medical insurance covers basic cataract surgery. The insurances generally do not cover Laser-Assisted Cataract Surgery or Advanced Technology Lens Implants.
Why is a lens implant needed during cataract surgery?
The cataract is the natural lens of the eye, which has lost its clarity. When the cataract is removed, there is no longer a lens inside the eye to focus light. An artificial lens implant is needed to provide focused vision.
How long do the lens implants last?
The lenses are permanently implanted inside the eyes and do not need to be replaced over time. So yes, they last forever! At Lee Eye Surgery Clinic, we only use high quality lens implants made by the top ophthalmic companies in the United States, no matter what type of lens implant the patient chooses.
Can the cataracts grow back?
No. Once the cataracts are removed, they do not grow back. A small percentage of patients can develop clouding of the capsule that holds the lens implant in place, causing blurred vision months to years after cataract surgery. This clouding of the capsule, called posterior capsular opacity, or PCO, can be easily treated with an outpatient laser procedure.
Will I need glasses after cataract surgery?
How often glasses are needed after cataract surgery will depend on the type of artificial lens that is implanted. Advanced Technology Intraocular Lenses can decrease your dependency of glasses by reducing astigmatism and providing focused distance, intermediate, and near vision.
How long does it take for the vision to recover after surgery?
While it takes the eyes a few weeks to completely heal from surgery, the patients can usually experience improvement in their vision within a few days to a week after surgery. Medication eyedrops are used before and after surgery to help the eyes heal.
Are there any restrictions after cataract surgery?
Modern cataract surgeries are performed through very small incisions compared to the past. Even though the risk of injuries are much lower than before, we do ask our patients to refrain from heavy lifting or prolonged bending for 1 week after surgery.
It is an abnormality in which the optical surfaces of the eye are shaped like a football (oval) rather than a baseball or basketball (round). Astigmatism is the most common optical problem after myopia (nearsightedness) and hyperopia (farsightedness).
How does astigmatism affect vision?
When it is uncorrected, astigmatism blurs vision at all distances, near and far.
How do I know if I have astigmatism?
There is no way of knowing without specific testing. Overall astigmatism is approximately the sum of what is in the cornea and what is in the lens. Cataract surgery eliminates the lens component of astigmatism. Any amount remaining in the cornea will contribute to reduced image quality without glasses following surgery. Some people have no astigmatism in their eyeglass measurements, yet they have astigmatism in their corneas. The only way of knowing if corneal astigmatism is present is to test for it.
What if I have no astigmatism or only a small amount?
Knowing there is little or no corneal astigmatism is just as important as knowing there is a lot because it determines how and where the surgeon places the incision for the lens surgery.
How is astigmatism corrected?
There are three methods. The first involves placing one or more incisions in the steep part of the peripheral cornea. The second involves modifying the length, depth or number of incisions. The third involves implanting a special intraocular lens, called a toric lens. The latter two approaches can be combined to achieve high amounts of astigmatism correction, if necessary.
What if I don’t have it corrected?
If you have residual astigmatism after surgery, there is a greater chance you will need glasses or contact lenses to see clearly. Your astigmatism can easily worsen after surgery if it is not measured before surgery and managed appropriately during surgery.
Are there other options?
The only other option is to perform your eye surgery without astigmatism correction and evaluate your astigmatism afterwards. Astigmatism can be corrected secondarily if you don’t like the initial result. However, this will require a second trip to the operating room, which will not be covered by Medicare or other health insurance. In this case, the cost will be 3 to 4 times higher than if you opted for astigmatism correction during the initial surgery. We are able to discount the cost at the time of initial surgery because we are already in the operating room.
Will I need astigmatism correction in both eyes?
Probably. The two eyes are often a little different. We evaluate them independently.
Will I see 20/20 if my astigmatism is corrected?
We hope so, but as with all surgery, we can’t guarantee outcomes. There are many variables that affect visual outcomes besides astigmatism (the power of the lens implant, the health of your retina and optic nerve, etc.). The odds of achieving 20/20 visual acuity without glasses or contact lenses are much better if we evaluate and correct your astigmatism than if we don’t.
Will it take longer to recover from surgery if my astigmatism is corrected?
Probably not. If you have a small amount of astigmatism, or a toric lens is implanted, recovery will be the same as usual. If the incision has to be lengthened, the eye might be a little more irritated the day after surgery. Either way, recovery is fairly quick.
Is it recommended for every patient?
If your potential vision is good, you should have your astigmatism evaluated and managed. Only if your potential vision is poor (because of advanced macular degeneration or some other eye problem), will correcting the astigmatism not be as beneficial.
Should I have my astigmatism corrected if my visual potential is poor?
It depends on your eye condition. If you won’t be able to see the big “E” on the eye chart after eye surgery, it really won’t help that much to have your astigmatism corrected.
Should I have my astigmatism corrected if I am having surgery in one eye only?
Yes. Your overall vision without glasses will be better even if only one eye is corrected.
What if my astigmatism is not fully corrected at the time of surgery?
You will still need glasses for best distance and near vision. Even if your astigmatism is not fully corrected, the quality of your uncorrected vision will be better if your astigmatism can be reduced by any amount. Refractive surgery (e.g. LASIK, PRK) can often be performed to further reduce astigmatism. Your surgeon will discuss which, if any, of these procedures is appropriate for your individual situation.
Will I need reading glasses if I have my astigmatism corrected?
If you opt to receive a monofocal lens implanted in both eyes for distance vision, you will definitely need reading glasses after surgery. If you opt for a multifocal lens implant (see the FAQs on Multifocal Intraocular Lenses) you may be able to see clearly in the distance and at near without glasses.
Are there any risks or side effects?
The only significant risk is that we won’t be able to correct all of your astigmatism, and you will need glasses or contact lenses for best vision.
Can I have surgery if I decide not to have my astigmatism corrected?
Yes you can, but this may result in a less-than-optimal result. State-of-the-art cataract and lens implant surgery involves correcting refracting errors at the time of surgery. You must elect Astigmatism Management if you wish to have a multifocal or accommodative lens implanted or if you wish to have monovision (monofocal implants in both eyes, one for distance and one for near vision). Astigmatism Management is of critical importance to optimize the performance of these lenses and improve your chance of being spectacle independent.
Does insurance (or Medicare) pay for astigmatism correction?
No, Medicare and other health insurance plans will not pay to reduce corneal astigmatism that exists at the time of cataract surgery.
Why doesn’t insurance (or Medicare) pay for astigmatism correction?
Medicare sets trends for the insurance industry. Since Medicare distinguishes between what is medically necessary and what is cosmetic, or purely optional, we are required to handle the cataract removal and the astigmatism management differently from the perspective of who pays. Medicare and private health insurance reimburse for cataract surgery. They do not pay for refractive surgery, which is necessary for astigmatism correction.
Can I submit the bill to insurance (or Medicare) for reimbursement after I pay?
Yes you can, but they will deny payment. If Medicare or an insurance company asks this office for justification for the astigmatism management, we will inform them the astigmatism correction was done for non-medical or cosmetic reasons.
Why do you charge for astigmatism correction?
Refractive cataract surgery is more involved than cataract surgery alone. It is costly and requires significantly more work to plan and perform than routine cataract surgery.
What is included in the astigmatism correction charge?
There are three components. First, we measure the amount of astigmatism in your cornea by obtaining a corneal topography map before and after surgery. The second component is astigmatism evaluation and surgical planning. This is a cognitive component that accounts for the bulk of the work. The third component is the surgical management. Astigmatic correction requires additional surgical steps.
Does astigmatism management require additional visits?
It is possible that your surgeon may wish to see you for an additional visit to assess the post operative stability of the astigmatism correction prior to surgery on the second eye.
Can I receive a refund if my astigmatism is not fully corrected?
No. As with any surgery, results are subject to individual healing patterns and a host of variables beyond our control. Generally speaking, if the amount of astigmatism remaining in the cornea after surgery is less than 1 diopter, a 20/20 uncorrected postoperative result is possible, barring any other ocular pathology. No guarantees can be made with respect to the final result.